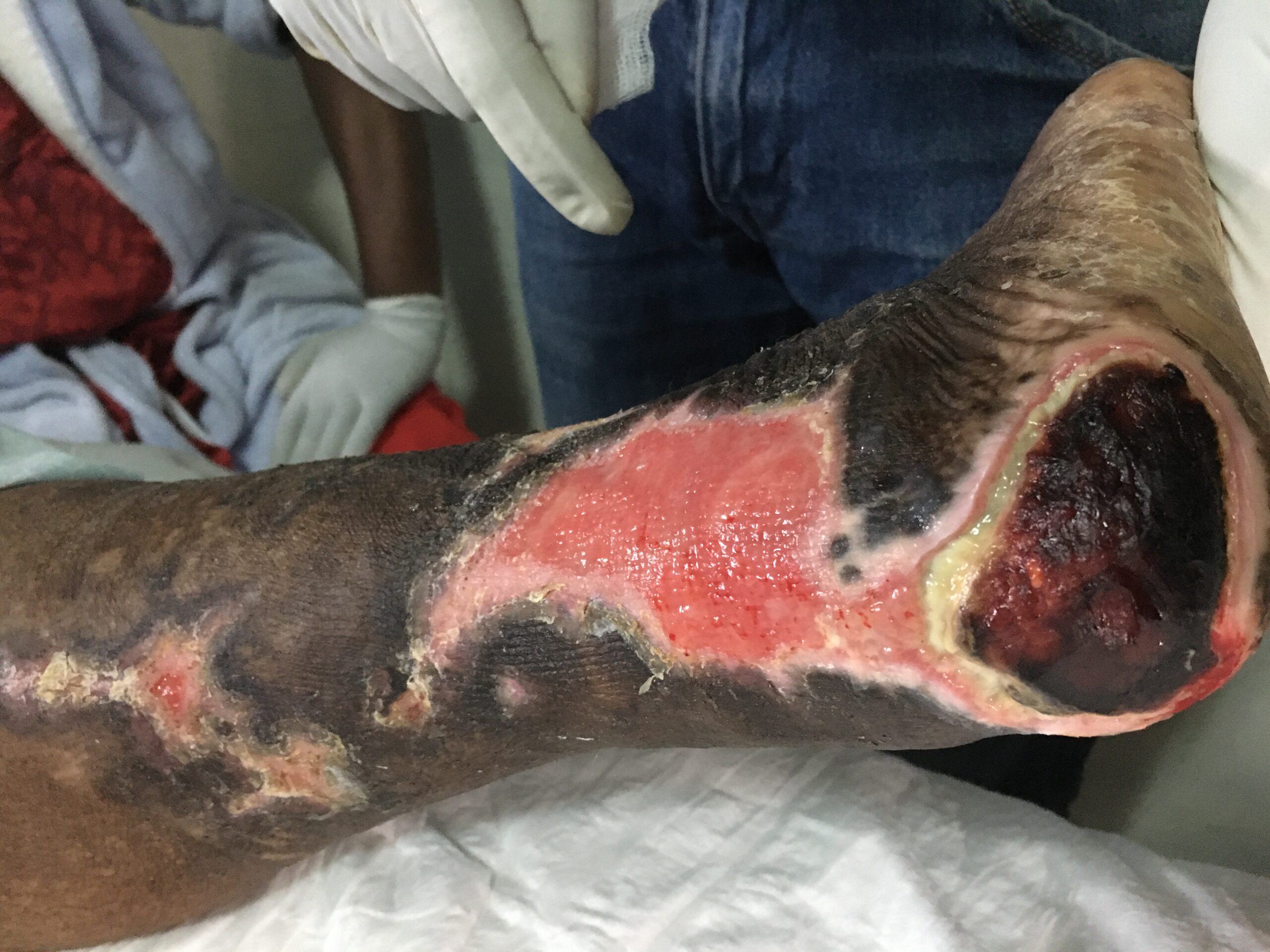
July marks No Amputation Month—a critical time to raise awareness about one of the most preventable causes of lower limb amputation: Diabetic Foot Ulcers (DFUs). These wounds, while common in individuals living with diabetes, are not inevitable. With proper education, timely intervention, and dedicated foot care, we can greatly reduce the risk of foot complications that often lead to limb loss.
At Stanley Wound & Ostomy Care, we believe that the best outcomes begin with knowledge, prevention, and early action.
Understanding the Burden of Diabetic Foot Ulcers
Globally, diabetic foot ulcers affect millions each year. Studies show that 19% to 34% of people living with diabetes will develop a foot ulcer during their lifetime. That means nearly 1 in 3 individuals with diabetes may face this complication if steps are not taken early.
According to recent evidence:
- The annual global incidence of diabetic foot ulcers is estimated between 9.1 million to 26.1 million cases.
- The prevalence among diabetic patients ranges from 2% to 12%, with an average global rate of 6.3%.
- Even more concerning, more than half (53.2%) of patients with diabetes are at risk of developing foot complications.
These figures are not just statistics—they represent real people whose mobility, independence, and quality of life are threatened.
Why Do Diabetic Foot Ulcers Occur?
DFUs don’t happen overnight. They usually begin with small changes in the feet that go unnoticed due to nerve damage (neuropathy) or poor circulation (ischemia). Without pain as a warning sign, patients may continue walking on a small blister, cut, or pressure point—causing the wound to deepen and become infected.
The most common risk factors include:
- Loss of protective sensation (due to peripheral neuropathy)
- Poor blood flow to the lower limbs
- Trauma—even minor injuries or ill-fitting shoes
- Uncontrolled blood sugar levels
- History of previous ulcers or amputations
When left untreated, a simple wound can turn into a life-threatening infection requiring hospitalization, surgery, or amputation.
What Can Be Done to Prevent Diabetic Foot Complications?
This month—and every month—we encourage all our patients with diabetes to take proactive steps to prevent foot ulcers and reduce their amputation risk. Here’s how you can stay a step ahead:
1. Inspect Your Feet Daily
Check for blisters, redness, cracks, swelling, or any unusual changes. If you can’t see the bottom of your feet, use a mirror or ask a loved one to help.
2. Never Ignore a Foot Wound
Even a small cut or blister should be treated seriously. Early treatment is the best way to avoid complications.
3. Wear Proper Footwear
Shoes should fit comfortably and protect your feet from pressure and injury. Avoid walking barefoot.
4. Control Your Blood Sugar
High blood glucose impairs healing and increases infection risk. Work with your healthcare provider to maintain optimal levels.
5. Schedule Regular Foot Exams
Professional foot assessments—especially by a wound care specialist—can identify early signs of risk before they progress to ulcers.
6. Seek Specialized Wound Care When Needed
If a wound does occur, early referral to a wound care specialist can drastically improve healing outcomes and reduce the need for amputation.
A Message of Hope and Empowerment
Every foot saved is a life changed. The truth is, most amputations caused by diabetic foot ulcers are preventable with timely and appropriate care. That’s why our team at Stanley Wound & Ostomy Care remains committed to walking alongside you—educating, treating, and supporting you through every step of your diabetes journey.
This No Amputation Month, let’s renew our commitment to foot health. Let’s make early care the standard and limb loss a rare exception.
If you or a loved one is living with diabetes, don’t wait for a wound to take you by surprise. Visit our clinic or call us today for a foot risk assessment and personalized care plan.