Introduction to Blast Injuries
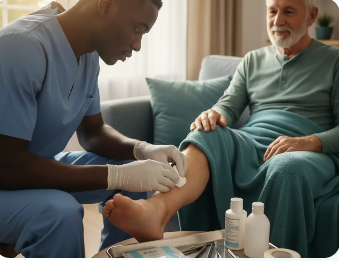
War has always been synonymous with destruction, chaos, and human suffering. Among the many medical challenges faced in battle, blast injuries stand out as some of the most devastating. Unlike a simple bullet wound or knife cut, blast trauma is complex—it’s not just one injury, but often a combination of multiple, life-threatening damages to the body. The human body is not designed to withstand the enormous pressure, heat, and shrapnel released by explosives. This makes blast injuries particularly unique in terms of both diagnosis and treatment.
Explosives have been used in wars for centuries, from early gunpowder cannons to the modern-day improvised explosive devices (IEDs). However, the impact on human bodies has remained tragically consistent: massive casualties, life-long disabilities, and overwhelming strain on healthcare systems. For soldiers, blast trauma often means losing limbs, hearing, or even cognitive functions. For civilians trapped in war zones, the suffering is even worse, as they lack access to proper medical care.
Understanding blast injuries is crucial not only for doctors and paramedics but also for policymakers, humanitarian organizations, and even regular citizens who live in regions affected by conflict. These injuries don’t just destroy bodies—they also leave behind scars that shape communities for decades.
Types of Blast Injuries
Blast injuries are not a single type of wound; they are classified into several categories depending on how the body is affected. Knowing these types helps doctors understand the mechanism of damage and provide the best possible treatment.
Primary Blast Injuries (Effect of Shock Waves)
The first and most direct impact of an explosion comes from the shock wave generated. When an explosive goes off, it creates a sudden and intense pressure wave that travels faster than sound. This wave moves through the air and directly hits the human body, especially hollow organs like the lungs, intestines, and ears.
Imagine blowing up a balloon until it bursts—now picture your lungs as that balloon. The force of the shock wave can rupture delicate tissues, leading to lung collapse, internal bleeding, or air embolism (air bubbles in the bloodstream that can block circulation). Eardrums are also highly sensitive to pressure changes, which is why hearing loss is one of the most common outcomes of primary blast injuries.
Secondary Blast Injuries (Shrapnel and Debris)
If the shock wave wasn’t deadly enough, the second phase of injury comes from flying debris. Explosives often contain metal casings or are placed in environments filled with stones, wood, or glass. When the bomb explodes, these fragments turn into high-speed projectiles, tearing through flesh and bone.
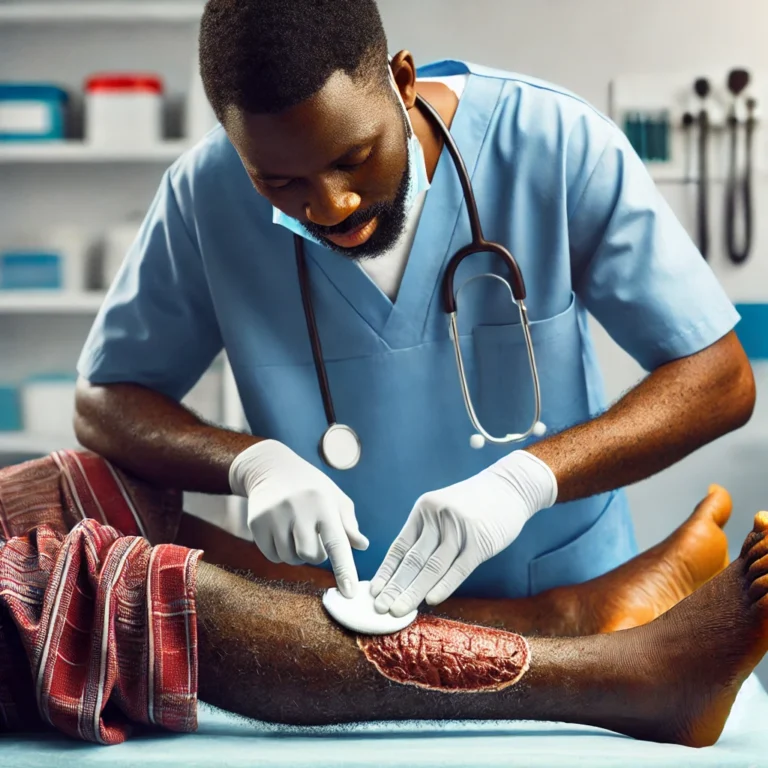
Secondary blast injuries are comparable to multiple gunshot wounds occurring simultaneously. Victims may have dozens of puncture wounds across their bodies, with fragments lodging deep inside muscles or organs. Removing this shrapnel often requires multiple surgeries, and in many cases, some fragments remain permanently inside the body.
Tertiary Blast Injuries (Body Displacement and Impact)
The blast wave not only pushes air but also propels bodies. Victims may be thrown against walls, vehicles, or even other people. These are called tertiary blast injuries. They often resemble blunt force trauma, with fractures, spinal injuries, or head trauma being common outcomes.
For instance, a soldier standing a few meters away from an explosion may not be pierced by shrapnel but could be thrown several feet into the air and land on concrete, suffering broken bones and brain injury. These injuries complicate treatment further, as doctors must distinguish between damage caused by direct impact and that caused by the blast wave itself.
Quaternary Blast Injuries (Burns, Inhalation Injuries, and Other Trauma)
Finally, there are the miscellaneous injuries grouped under quaternary blast trauma. These include burns from the fireball, inhalation injuries from smoke and toxic gases, and even crush injuries if buildings collapse after the blast.
Unlike the other categories, quaternary injuries are highly variable and depend on the environment of the explosion. In an urban setting, victims may suffer from dust inhalation leading to long-term lung disease, while in open battlefields, severe burns are more common.
The combination of these four types makes blast trauma uniquely complex. A single patient may simultaneously have a collapsed lung, multiple shrapnel wounds, a broken leg, and severe burns—all of which require urgent, specialized treatment.
Pathophysiology of Blast Injuries
To truly grasp why blast injuries are so destructive, it’s important to understand how blast waves interact with the human body.
When an explosive detonates, it releases energy in a fraction of a second. This produces an initial over-pressurization wave (the blast wave) followed by a negative pressure phase (the suction effect). Human tissues, especially those containing air, are extremely vulnerable to these rapid pressure shifts.
The lungs are the most affected organ. The alveoli (tiny air sacs) rupture under extreme pressure, leading to pulmonary hemorrhage or acute respiratory distress. The brain is also highly sensitive; blast waves can cause concussions or traumatic brain injuries even without visible head wounds. This explains why many soldiers exposed to IEDs suffer from cognitive issues later in life.
The ears are often the first casualty. The eardrum ruptures at relatively low pressures, causing temporary or permanent hearing loss. This explains why ringing in the ears (tinnitus) is a common complaint after explosions.
Another vulnerable system is the gastrointestinal tract. Blast waves can rupture intestines, causing internal bleeding and infections that may not show immediate symptoms but become life-threatening within hours.
Interestingly, studies show that blast trauma differs between military personnel and civilians. Soldiers are often equipped with protective gear, reducing shrapnel injuries but not fully protecting them from pressure waves. Civilians, however, are usually unprotected and thus suffer more from secondary and quaternary injuries, making their survival rates much lower.
Diagnosis and Assessment
In war zones, diagnosing blast injuries is extremely challenging. Unlike simple trauma cases, blast victims often appear deceptively stable at first, only to collapse later from hidden internal injuries
Immediate Field Assessment of Blast Victims
The first step is always airway, breathing, and circulation (the ABCs of trauma care). Field medics must quickly identify life-threatening conditions like collapsed lungs, uncontrolled bleeding, or traumatic amputations.
Role of Imaging and Medical Technology in Diagnosing Injuries
In advanced hospitals, CT scans and ultrasounds help identify internal damage. However, such equipment is often unavailable in war zones, leaving doctors dependent on clinical signs and experience.
Challenges of Diagnosing Internal Damage in Resource-Limited War Zones
The lack of proper facilities often leads to delayed diagnoses. For example, a soldier may walk into a field hospital appearing fine but collapse hours later due to undetected internal bleeding. This makes blast injuries particularly deadly in remote or resource-poor environments.
Emergency Management of Blast Injuries
When it comes to saving lives after explosions, time is the most critical factor. The golden hour—the first 60 minutes after trauma—is where most lives can be saved if proper care is given.
First Aid and Stabilization in the Field
Basic first aid like applying tourniquets, sealing chest wounds, and giving oxygen can dramatically improve survival chances. Soldiers are often trained to provide self-aid or buddy aid, which has saved countless lives in recent conflicts.
Triage Systems for Mass Casualty Events
In large-scale explosions, not every victim can be treated immediately. Triage systems classify patients into categories: those who need immediate surgery, those who can wait, and those unlikely to survive even with treatment. This grim reality ensures resources are used effectively in mass casualty events.
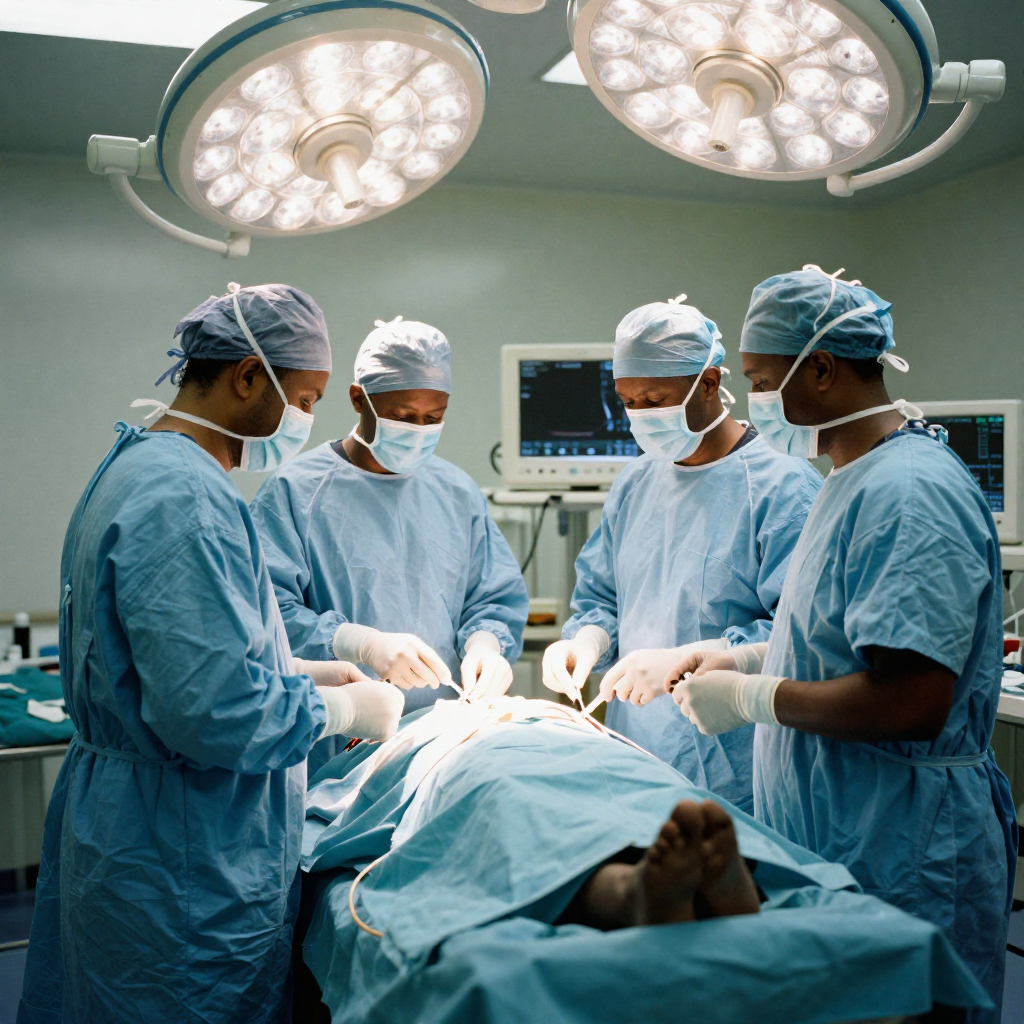
Surgical Interventions in Blast Trauma Patients
Surgery for blast victims is often complex. Amputations are common due to shredded limbs, while abdominal surgeries are needed for internal bleeding. Neurosurgeons may be required for traumatic brain injuries, though such specialists are rarely available in war zones.